Arthrosis of the hip joint is a degenerative-dystrophic pathology, which is characterized by the destruction of hyaline cartilage.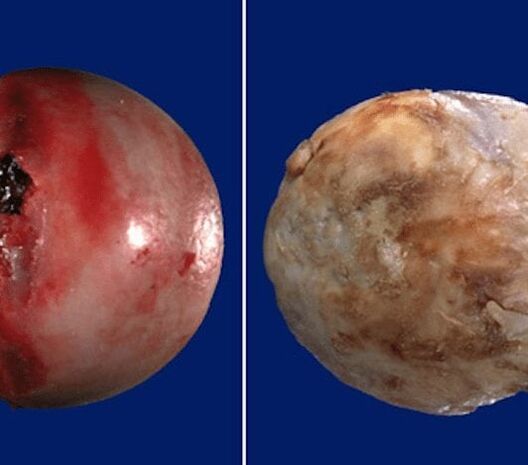 The disease develops gradually, accompanied by pain and decreased range of motion. In the absence of medical intervention in the initial phase of arthrosis, after a few years, atrophy of the femoral muscles occurs.
The disease develops gradually, accompanied by pain and decreased range of motion. In the absence of medical intervention in the initial phase of arthrosis, after a few years, atrophy of the femoral muscles occurs.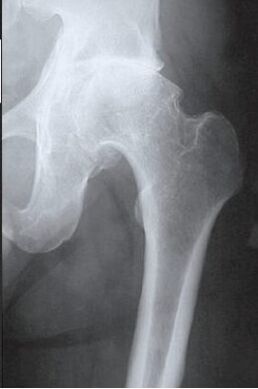 The injured limb is shortened and the fusion of the joint space leads to partial or complete immobilization of the hip joint. The causes of the pathology are previous injuries, spinal curvature, systemic diseases of the musculoskeletal system.
The injured limb is shortened and the fusion of the joint space leads to partial or complete immobilization of the hip joint. The causes of the pathology are previous injuries, spinal curvature, systemic diseases of the musculoskeletal system.
Osteoarthritis is usually detected in middle-aged and elderly patients. The diagnosis is made based on the results of instrumental studies - radiography, magnetic resonance, computed tomography, arthroscopy. The treatment of pathologies of 1 and 2 degrees of severity is conservative. If ankylosis is detected or drug therapy is ineffective, a surgical operation (arthrodesis, endoprosthesis) is performed.
The pathology development mechanism
The hip joint is made up of two bones - the ilium and the femur. The lower part of the ilium is represented by its body, which participates in the articulation with the femur, forming the upper part of the acetabulum. During the movement, the glenoid fossa is immobile and the femoral head moves freely. This "hinge" device of the hip joint allows it to bend, unfold, rotate, promote abduction, adduction of the hip. The smooth, resilient and resilient hyaline cartilage that lines the acetabulum and the femoral head provides unimpeded sliding of the articular structures. Its main functions are the redistribution of loads during movement, preventing rapid wear and tear of bone tissues.
Under the influence of external or internal factors, cartilage trophism is disturbed. It does not have its own circulatory system - synovial fluid provides nutrients to the tissue. In arthrosis, it thickens, becomes viscous.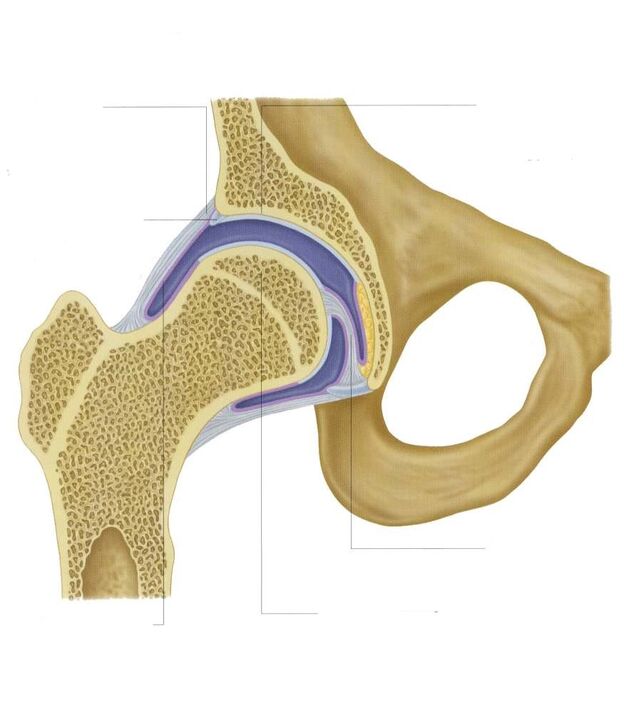 The resulting nutrient deficiency causes the surface of the hyaline cartilage to dry out. It is covered by cracks, which leads to permanent microtrauma of the tissues during flexion or extension of the hip joint. Cartilage gets thinner and loses its cushioning properties. The bones are deformed to "adapt" to the increased pressure. And in the context of deteriorating tissue metabolism, destructive and degenerative changes progress.
The resulting nutrient deficiency causes the surface of the hyaline cartilage to dry out. It is covered by cracks, which leads to permanent microtrauma of the tissues during flexion or extension of the hip joint. Cartilage gets thinner and loses its cushioning properties. The bones are deformed to "adapt" to the increased pressure. And in the context of deteriorating tissue metabolism, destructive and degenerative changes progress.
Causes and provocative factors
Idiopathic or primary arthrosis develops for no reason. It is believed that the destruction of cartilaginous tissue occurs due to the natural aging of the body, slowing down the recovery processes, decreased production of collagen and other compounds necessary for the full regeneration of the structures of the hip joint. Secondary arthrosis occurs in the context of a pathological condition already present in the body. The most common causes of secondary disease include:
- previous injuries - damage to the ligament-tendon system, muscle ruptures, its complete separation from the bone base, fractures, dislocations;
- violation of joint development, congenital dysplastic disorders;
- autoimmune pathologies - rheumatoid, reactive, psoriatic arthritis, systemic lupus erythematosus;
- non-specific inflammatory diseases, such as purulent arthritis;
- specific infections - gonorrhea, syphilis, brucellosis, ureaplasmosis, trichomoniasis, tuberculosis, osteomyelitis, encephalitis;
- disruption of the functioning of the endocrine system;
- degenerative-dystrophic pathologies - osteochondropathy of the femoral head, osteochondritis dissecans;
- hypermobility of the joints, due to the production of "superextensible" collagen, causing its excessive mobility, weakness of the ligaments.
Since the cause of the development of osteoarthritis may be hemarthrosis (hemorrhage in the hip joint cavity), the triggering factors include disorders of hematopoiesis. The prerequisites for the onset of the disease are overweight, excessive physical activity, sedentary lifestyle. Its development is caused by an inadequate organization of sports training, a deficiency in the diet of foods with a high content of microelements, fat-soluble and water-soluble vitamins. Postoperative arthrosis occurs several years after surgery, especially if it is accompanied by the excision of a large amount of tissue. Hyaline cartilage trophism is disturbed with frequent hypothermia, living in an environment that is unfavorable to the environment and working with toxic substances.
Arthrosis of the hip joint cannot be inherited. But in the presence of certain congenital characteristics (metabolic disorders, skeletal structure), the likelihood of their development increases significantly.
Symptoms
The main symptoms of osteoarthritis of the hip joint are pain when walking in the hip region, radiating to the groin, knee joint. A person suffers from stiffness of movement, stiffness, especially in the morning. To stabilize the joint, the patient begins to limp, his gait changes. Over time, due to muscle atrophy and joint deformation, the limb becomes visibly shortened. Another characteristic sign of pathology is the limitation of hip abduction. For example, difficulties arise when trying to sit on a stool with your legs apart.

For first-degree arthrosis, periodic pain occurs after intense physical exertion. They are located in the joint area and disappear after a long rest.
With second-degree arthrosis of the hip joint, the severity of the pain syndrome increases. The discomfort occurs even at rest, extends to the thigh and groin, increases with weight lifting or increased motor activity. To eliminate pain in the hip joint, the person starts limping almost imperceptibly. Limitation of movement in the joint is observed, especially during abduction and internal rotation of the thigh.
Third-degree arthrosis is characterized by intense and constant pain, which does not subside during the day and night. The difficulty in locomotion arises, therefore, when walking, the person is forced to use a cane or crutches. The hip joint is rigid, there is significant atrophy of the muscles of the buttocks, thighs and legs. Due to the weakness of the abductor femoral muscles, the pelvic bones are displaced in the frontal plane. To compensate for the shortening of the leg, the patient leans towards the injured limb when moving. This causes a strong change in the center of gravity and an increase in the tension in the joint. At this stage of arthrosis, pronounced ankylosis of the joint develops.
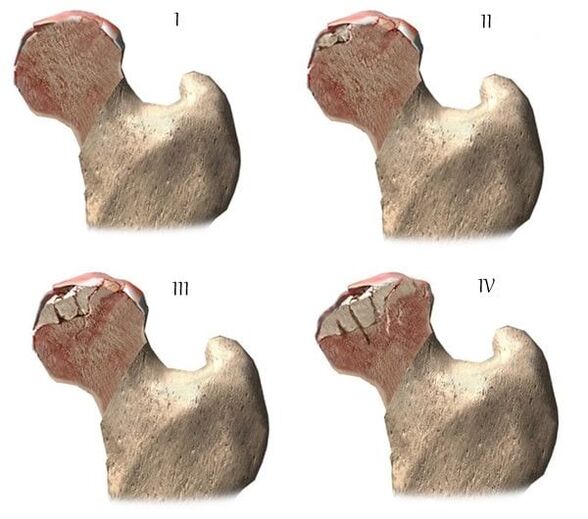
| Degrees | Radiographic signs |
| The first | The changes are not pronounced. The articular gaps are moderately unevenly narrowed, there is no destruction of the surface of the femur. Small bone growths are observed at the outer or inner edge of the acetabulum |
| The second | The height of the joint space is significantly reduced due to its uneven fusion. The bony head of the femur is displaced upwards, deformed, dilated, its contours become irregular. Bone growth forms on the surface of the inner and outer edges of the glenoid fossa |
| Third | There is a complete or partial fusion of the joint space. The femoral head is strongly extended. Multiple bone growths are located on all surfaces of the acetabulum |
Diagnosis
When making a diagnosis, the doctor takes into account the clinical manifestations of the pathology, the anamnesis, the results of an external examination of the patient and instrumental studies. Radiography is the most informative. With its help, the condition of the hip joint is evaluated, the stage of its course, the degree of damage to the cartilaginous tissues and, in some cases, the cause of development is established. If the cervical-difisary node is enlarged and the acetabulum is oblique and flattened, then with a high degree of probability it is possible to assume congenital dysplastic changes in the joint. Perthes' disease or juvenile epiphysiolysis is indicated by the altered shape of the hip bone. Radiography can reveal post-traumatic arthrosis, despite the absence of previous trauma in the anamnesis. Other diagnostic methods are also used:
- CT helps to detect the growth of the edges of bone plates, formed osteophytes;
- Magnetic resonance imaging is performed to assess the condition of connective tissue structures and the degree of their involvement in the pathological process.
If necessary, the internal surface of the joint is examined with arthroscopic instruments. The differential diagnosis is made to exclude gonarthrosis, lumbosacral or thoracic osteochondrosis. Arthrosis pain can be disguised as clinical manifestations of root syndrome caused by compression or inflammation of the nerve. It is usually possible to exclude neurogenic pathology with the help of a series of tests. Arthrosis of the hip joint is necessarily differentiated from trochanteric bursitis of the hip joint, ankylosing spondylitis, reactive arthritis. To exclude autoimmune pathologies, biochemical studies of blood and synovial fluid are performed.
Drug treatment tactics
Medical treatment aims to improve the patient's well-being. For this, medicines from different clinical and pharmacological groups are used:
- non-steroidal anti-inflammatory drugs (NSAIDs) - Nimesulide, Ketoprofen, Diclofenac, Ibuprofen, Meloxicam, Indomethacin, Ketorolac. To relieve acute pain, injectable solutions are used and tablets, pills, ointments, gels help to eliminate pain of mild or moderate severity;
- glucocorticosteroids - Triamcinolone, Dexamethasone, Hydrocortisone. They are used in the form of intra-articular blocks in combination with the anesthetics Procaína, Lidocaína;
- muscle relaxants - Baclofen, Tizanidine. They are included in treatment regimens for skeletal muscle spasms, pinching of sensitive nerve endings;
- drugs that improve blood circulation in the joint - nicotinic acid, aminophylline, pentoxifylline. Patients are prescribed to improve tissue trophism, prevent disease progression;
- chondroprotectors. Effective only in stages 1 and 2 of arthrosis.
Rubbing ointments with a heating effect helps to eliminate mild pain. The active ingredients of external agents are capsaicin, cinquefoil, camphor, menthol. These substances are characterized by an irritating, distracting and local analgesic effect. Compresses joints with Dimethylsulfoxide, the medical bile that helps to deal with swelling, the morning swelling of the thigh. Patients are recommended for classical coxarthrosis, acupressure or vacuum massage. Daily exercise therapy is an excellent prevention of the progression of osteoarthritis.
Surgical intervention
With the ineffectiveness of conservative therapy or the diagnosis of a pathology complicated by ankylosis, an operation is performed. It is impossible to restore the cartilaginous tissue of the joint damaged by osteoarthritis without prosthetic surgery, but with the correct treatment approach, adherence to all medical prescriptions, maintaining a correct lifestyle, performing therapeutic exercises, regular massage courses, taking vitaminsand proper nutrition, you can stop the process of injury and destruction of the cartilage and hip joints.






















